Pes planus or pes plano valgus are medical terms for flat feet and the associated weight bearing position of the foot. The main supportive structure of the foot is the arch. Pes planus may be diagnosed if the arch is flattened or absent. Pes planus may be noted early in life and in this case it is considered to be congenital pes planus. The condition may also be acquired due to inheritance of poor foot mechanics, trauma/over-use, conditions involving impaired collagen synthesis (Ehlers-Danlos syndrome, Marfan’s syndrome), rheumatoid arthritis, neurologic disorders and neuromuscular disorders, pregnancy, and obesity. An individual may have flexible flat feet or rigid flat feet. The majority of the cases are flexible. This means that the arch can be recreated by manual manipulation or by standing on one’s toes. Rigid flat feet may be the result of a congenital condition, trauma, and late stages of neuroarthropathy among other reasons.
The significance of pes planus has been debated throughout the years amongst practitioners of various specialties. It is true that many individuals with flat feet do not experience any functional disadvantage or any symptoms; however, some people with pes planus are prone to foot/ankle/knee/hip/back pain, foot fatigue/cramping, and other associated deformities such as bunions and hammer toes. Bone and joint instability are compromised as well as the function of certain muscles and tendons. This is especially true if the feet overpronate (pes plano valgus). Supination and pronation are both necessary rotational movements that the foot undergoes during the gait (walking) cycle; however, some individuals may pronate too much or too little. The level of activity, the type of activities, and the degree of standing and walking daily seem to correlate to the development of symptoms associated with flat feet.
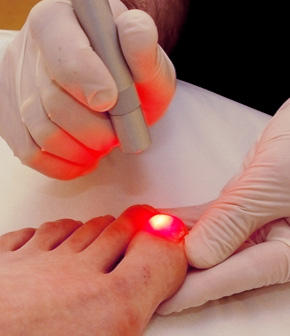
Diagnosis is made based on the history and clinical exam. Sometimes x-rays and other diagnostic tests such as MRI are performed to diagnose secondary conditions related to pes planus. Non-surgical treatment involves strapping and arch supports or orthotics (inserts for shoes) which may be over the counter or custom made. Your doctor will determine if soft, semi-flexible, or rigid inserts are appropriate. He or she can also determine if custom orthotics are indicated. Orthotics are designed to support and align the feet. Not everyone is a candidate for orthotics, particularly those whose feet fall into the rigid category. Orthotics function similarly to eyeglasses or hearing aids. They will not cure the condition, but they can correct or manage the condition while they are being used. Supportive shoes and sneakers are also recommended.
Surgery is recommended only as a last resort when all possible non-surgical options have been exhausted. Surgery may involve reinforcing tendons, correcting the alignment of bones and joints, or a combination of both.