Plantar fasciitis is an inflammation of the plantar fascia of the foot. The plantar fascia is a thick band of fibrous connective tissue that connects the heel to the ball of the foot and the base of the toes. The underside of the foot is the plantar aspect of the foot. The plantar fascia is responsible for supporting the arch. The fascia has the ability to stretch to a certain degree each time the foot impacts the ground. The condition occurs when the plantar fascia is stretched beyond the degree to which it is accustomed causing strain and possibly partial tears of its fibers. Over time this leads to inflammation, pain, and possibly the development of a heel spur. A heel spur is an extension or protrusion of the heel bone. When the plantar fascia is strained it can repeatedly tear away the lining or tissue that covers the heel bone resulting in a spur. Plantar fasciitis and heel spur syndrome are terms that are often used interchangeably. It is important to understand that individuals with heel spurs may never develop plantar fasciitis or heel pain, and individuals suffering from plantar fasciitis may never develop a heel spur. The presence of a spur does not commonly change the treatment as it is not the primary cause of pain.
About 90% of the time plantar fasciitis is the cause of heel pain. Heel pain also manifests with a traumatic fracture, a stress fracture, a bone tumor, a bone bruise, Achilles tendon related bursitis, neuritis, and Sever’s apophysitis (irritation of the growth plate seen in children). History, physical exam, radiographs, and sometimes an MRI will determine the cause of the pain.
Plantar fasciitis can occur in one foot or both. Multiple factors can contribute to its development. Some of these factors include certain types of activities, a sudden increase in activity, an occupation that involves continued standing or walking, shoes/sneakers that lack sufficient support, weight gain, pregnancy, inherited poor foot mechanics, flat feet, and high arched feet.
Symptoms manifest as pain located at the inside of the heel and/or the bottom of the heel. Pain is usually worse in the morning after getting out of bed and after periods of non weight bearing such as after a drive or after being seated for a while. The pain tends to ease up after a few minutes, but may not completely disappear. It may be intense at the end of the day as well. Individuals who have been suffering with the condition for several months may experience discomfort constantly. Commonly, the heel does not appear to be discolored or swollen.
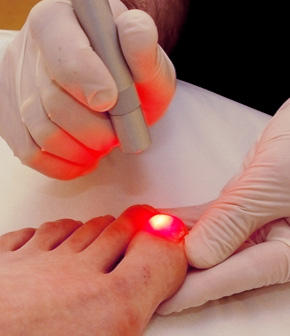
Treatment involves multiple modalities. Patients should be aware that the condition can linger for many months even after implementing a treatment program. Treatment may include oral medication, injection therapy, ice, particular stretching exercises, physical therapy, strapping, night splints, arch supports or custom orthotics, modifying shoes, and rest from certain activities. Treatment must be twofold. It must be aimed at both eliminating the inflammation as well as addressing the source of the condition to prevent recurrence.